Most readers who come across this text ask one of two questions: can a marten in the attic infect me with rabies, or — worse — I've just been scratched / bitten, what now. Short answer to the first: the risk in Poland in 2026 is low, but not zero. Short answer to the second: regardless of everything, go to the ER or the nearest rabies vaccination point. You'll find the rest — facts, a map, the procedure — below.
This text is for informational purposes and is based on data from the General Veterinary Inspectorate, WHO, OIE, and Polish clinical practice. It is not a substitute for medical advice. Any suspected exposure to rabies — involving a marten, fox, raccoon dog, bat, or other wild mammal — requires consultation with a physician and notification to the State Sanitary Inspection. If you are unsure which animal you are dealing with, start with the text Marten vs. Weasel — What's Worth Knowing.
§ 01What is Rabies — The Virus and Foundations
Rabies (rabies) is an acute, progressive disease of the central nervous system caused by viruses of the genus Lyssavirus from the family Rhabdoviridae. The classic etiological agent — RABV (Rabies Lyssavirus) — is responsible for most cases worldwide. In Europe, bat variants (EBLV-1 and EBLV-2) also circulate, which are epidemiologically distinct from the terrestrial type.
The mechanism is always the same. The virus enters the body along with the saliva of an infected animal — most often through a bite wound, less frequently through contact of saliva with damaged skin or mucous membranes. After exposure, an incubation period follows (usually 20–90 days, but both several-day and multi-year periods have been described). During this time, the virus travels along nerve endings to the spinal cord, and from there to the brain. Once it reaches the CNS and clinical symptoms appear — it is already too late.
The effectiveness of treatment after symptoms appear in humans is practically zero. Only a dozen or so documented survivals have been recorded worldwide after the full clinical picture, most with severe neurological consequences. Therefore, the entire medical approach is based on post-exposure prophylaxis (PEP) — starting vaccination and, if indicated, immunoglobulin before the virus manages to reach the nervous system.
This article is not a substitute for medical advice or veterinary diagnostics. Any suspected contact with rabies in a human — bite, scratch, contact of saliva with cut skin — requires immediate notification to the nearest ER, rabies vaccination point, or District Sanitary-Epidemiological Station. Any suspicion in an animal (wild or domestic) should be reported to the District Veterinary Officer. These are free, legally available pathways.
§ 02The Situation in Poland — Since When Foxes Have Been Vaccinated
Poland has been conducting mass oral vaccination of wild foxes continuously since 1993. The program involves distributing baits containing a live attenuated vaccine (most often the SAD B19 or SAG-2 strain) from aircraft and by hand. The campaign is conducted twice a year — in spring and autumn — by the Veterinary Inspection with the participation of the Polish Hunting Association.
The effect is measurable and spectacular. In the mid-1990s, 2,000–3,000 cases of rabies per year were recorded in animals in Poland, almost throughout the country. After two decades of systematic vaccinations, this number has dropped to several dozen a year, and for several years it has remained within the range of several to a dozen cases per year, limited mainly to border regions with eastern neighbors.
At the international level, since 2013, Poland has had the status of a country territorially free of rabies in wild terrestrial animals with respect to most provinces, according to the WHO/OIE classification (now WOAH). The status is not uniform — individual eastern provinces periodically lose it after outbreaks are detected and regain it after two years without new cases.
| Period | Annual cases in animals | Epidemiological status |
|---|---|---|
| 1980s | 2,500–3,500 | endemic throughout the country |
| 1993 | vaccination start | first oral campaign for foxes |
| 2000–2010 | 200–800 | gradual decline, regionalization |
| 2013 | several dozen | WHO: territorially free status |
| 2020–2026 | several–a dozen | outbreaks mainly in the east |
Recent outbreaks have occurred in the following provinces: Masovian, Lublin, Subcarpathian, Podlaskie, and Lesser Poland. They most often concerned foxes and raccoon dogs — introduced from non-EU territories — and, occasionally, domestic animals in direct contact with a sick wild predator. Every detection triggers a procedure: area quarantine, intensive vaccinations, and taking samples from dead animals.
§ 03Can a Marten Get Rabies?
Short answer: yes, but rarely. Rabies can affect any mammal, including the stone marten (Martes foina), pine marten (Martes martes), and least weasel (Mustela nivalis). A longer answer requires distinguishing between three concepts: susceptibility, role as a reservoir, and role as a vector.
- Susceptibility — the marten is susceptible to infection. If bitten by a sick fox or raccoon dog, the probability of falling ill is real. In this respect, it is no different from a dog, cat, or even a human.
- Reservoir — in Poland and throughout Central Europe, the reservoir of terrestrial rabies is primarily the red fox (Vulpes vulpes), and to a lesser extent, the raccoon dog (Nyctereutes procyonoides). The marten does not independently maintain the circulation of the virus in the population — a marten population without contact with foxes and raccoon dogs would quickly rid itself of the virus.
- Occasional vector — a single sick marten could theoretically bite a human or a domestic animal and pass the virus on. These are statistically marginal events, but not zero. In the last 15 years in Poland, isolated laboratory-confirmed cases of rabies in martens have been recorded, always in areas with an active outbreak among foxes.
In numbers: out of about 10 cases of rabies detected annually in animals in Poland, over 90% are foxes and raccoon dogs. The rest are (in order): bats (with a separate EBLV variant), domestic dogs and cats (usually unvaccinated, in the outbreak area), badgers, and martens — sporadically, once every few years. Statistics clearly indicate where the real risk lies.
The marten in Poland is not a reservoir for rabies. It is its potential victim — and very rarely, in an area of an active outbreak, its occasional vector.
From the perspective of a house inhabitant whose attic is hunted by a stone marten, this means more or less this: statistically, the risk of rabies from this specific marten is close to zero if you live in a western or central province and do not observe symptoms of disease in it. The question carries different weight if you live in the Lublin region, near the eastern border, and an outbreak in foxes has just been detected. Geographical context changes everything. More about the species itself in the text Pine Marten vs. Stone Marten.
§ 04How to Recognize a Sick Marten
Rabies in mustelids — as in foxes — takes two forms: furious (aggressive form) and dumb (paralytic form). It often starts with the first and transitions into the second within a few days. For a person observing the animal from a safe distance, the most important thing is not to confuse diseased behavior with the normal daytime passage of a healthy marten.
Martens in Poland, especially urban stone martens, are sometimes seen during the day — and this alone does not indicate anything dangerous. An alarm signal begins with the combination of several symptoms at once.
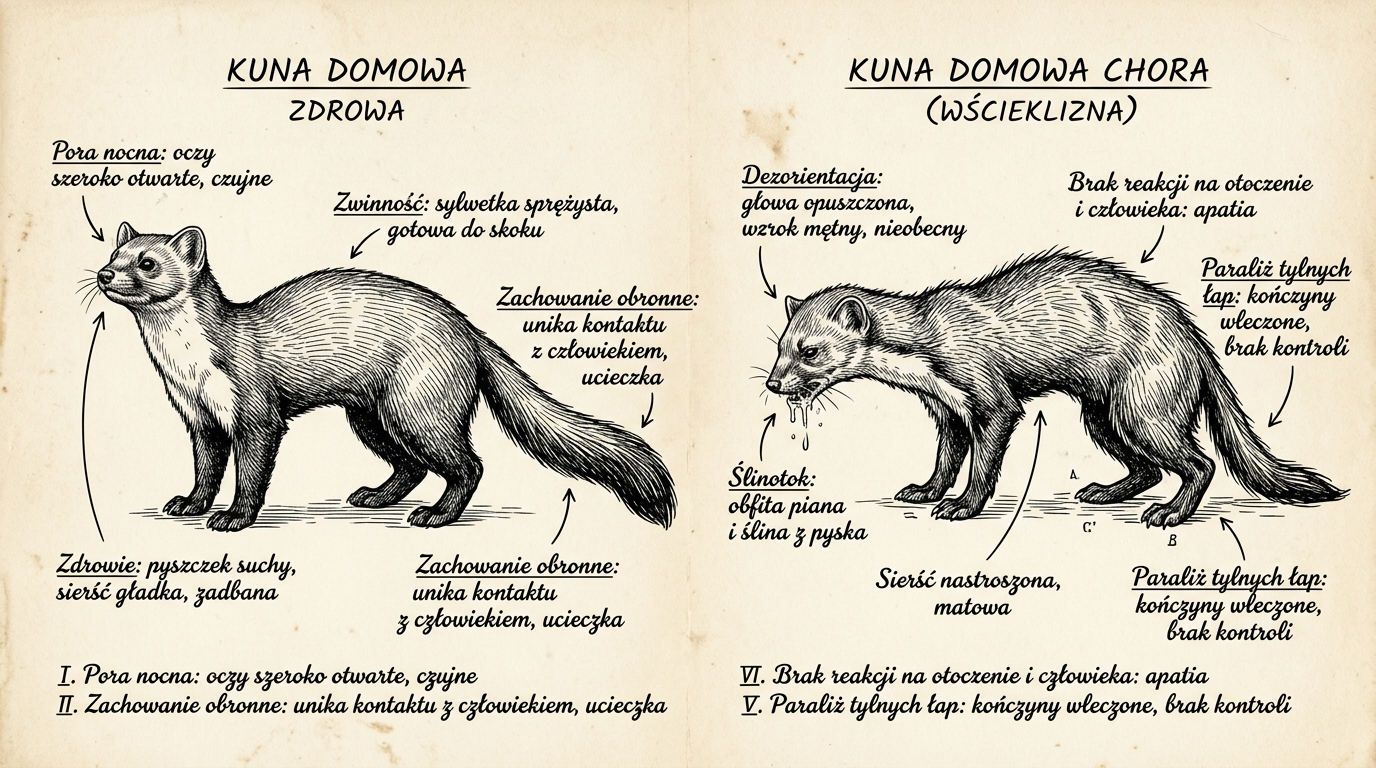
| Feature | Healthy marten | Sick marten (suspected) |
|---|---|---|
| Daily activity | mainly dusk and night, occasionally at dawn | in full sun, midday hours |
| Reaction to humans | immediate flight, distance | no flight, comes close, does not react |
| Movement | fluid, springy, quick jumps | stumbling, uncertain gait, paralysis of hind legs |
| Muzzle and saliva | dry, clean | drooling, foam, drooping jaw |
| Voice | huffing, hissing when threatened | spontaneous vocalization, groans, howls, voicelessness |
| Behavior | secretive, alert, investigative | aggression without provocation or apathy / disorientation |
A single feature is not enough for suspicion. A marten stumbling from hunger or after being hit by a car does not have rabies. A marten observed at noon, a marten aggressively defending its young — also not. The signal is only when three elements combine: activity at an unusual time, lack of normal distance from humans, and neurological symptoms (drooling, ataxia, paralysis).
Do not approach. Do not try to catch it, do not provide water or food, do not let children or pets approach. Call the District Veterinary Officer (every province has a list online) or 112, provide the location and observed symptoms. If the marten is dead — do not touch the carcass, mark the place, report through the same channels. The Veterinary Inspection will take a sample for laboratory testing for rabies.
§ 05What to Do After Contact or a Bite
The most important rule is this: with every exposure to potentially infectious saliva, every bite and scratch with skin breakage, report immediately to a doctor. Do not wait "to see if it hurts." Do not wait "until it heals." The decision on post-exposure prophylaxis is made based on risk assessment, not after symptoms appear — because then it is already too late.
Procedure, step by step:
- Step 1 — immediate washing of the wound for at least 15 minutes. Running water with soap, vigorously, not sparing the wound. This sounds trivial, but it is one of the best-documented interventions reducing the risk of infection (mechanically removing a significant portion of virus particles). After washing — wipe the skin with an antiseptic preparation (iodine, 70% alcohol, octenidine).
- Step 2 — immediate contact with the ER or vaccination point. Rabies prophylaxis points are located in every province (list on the GIS website). Do not delay until the next day. The decision on vaccination and possible immunoglobulin will be made by a doctor based on the WHO exposure category (I, II, III).
- Step 3 — describe the event exactly: animal species (if identified), behavior (typical / atypical), circumstances of contact, region. If the animal was caught or died — information on where it is located is critical for veterinary services. Species identification is aided by the text Animals Similar to Martens.
- Step 4 — sanitary-epidemiological notification. The doctor fills out the form reporting suspected infectious disease to the State Sanitary Inspection (form ZLK-1). You will receive a vaccination schedule (5-dose Essen or 4-dose Zagreb scheme) and, if indicated, rabies immunoglobulin injected around the wound.
- Step 5 — observation of the animal (if it is a dog or cat with a known owner). In the case of a bite by a known domestic dog/cat with a vaccination document, the doctor may recommend 10-day veterinary observation instead of immediate full PEP. For wild animals — this option does not exist.
PEP, including vaccinations and immunoglobulin, is free for any person with exposure to suspected rabies, regardless of insurance. It is funded by the state budget as part of the Ministry of Health's tasks. The only thing you must not do is not report because of cost concerns. Every ER has an obligation to admit and start the pathway.
§ 06Map of Rabies Outbreaks in Poland
The Veterinary Inspection maintains an updated map of rabies outbreaks in animals in Poland, available publicly on the website of the General Veterinary Inspectorate and in EU systems (ADIS, Animal Disease Information System). Data is updated weekly, divided by species, province, district, and date of laboratory confirmation.
The geographical structure of risk in Poland in 2026 is quite clear:
- Western and central provinces (Lubusz, Greater Poland, Lower Silesian, Opole, Łódź, Kuyavian-Pomeranian, Pomeranian, western Masovian) — for several years no new outbreaks in wild animals, territorially free status. Risk of exposure close to zero in daily conditions.
- Eastern provinces (Podlaskie, Lublin, Subcarpathian, partially Lesser Poland and eastern Masovian) — sporadic outbreaks, most often in foxes and raccoon dogs introduced from Belarus and Ukraine. Here, there are periodically intensified oral vaccination campaigns and increased surveillance.
- Border zones — a 50 km strip from the eastern border treated as a buffer area, with additional vaccination campaigns conducted by the Veterinary Inspection together with EU partners.
- Bat rabies (EBLV) — isolated cases throughout Poland, statistically marginal, but taken into account with every contact with a bat (every such event is treated as category III exposure).
Practical advice before going into the field: check the GIWET map for the specific district you are going to for vacation, to a homestead, or an allotment. If an outbreak has been recorded there in the last 6 months — it does not significantly change daily behavior, but it's worth making sure the dog has had a fresh vaccination and children know that we do not approach any wild animal, no matter how cute it looks. This is a rule that costs nothing and works absolutely every time.
§ 07Prevention and Vaccination of Dogs and Cats
In this entire conversation about martens, the most sensible thing you can do as a resident of a property visited by wild predators is to keep your own animals' vaccinations up to date. This buffers the risk regardless of whether there are martens, foxes, raccoon dogs, or bats in the area.
- Dogs — mandatory vaccination under Art. 56 of the Act of March 11, 2004, on Animal Health Protection. First vaccination — between 12 and 16 weeks of age, booster dose annually or every 2–3 years depending on the preparation (as recommended by the veterinarian). Lack of vaccination = fine and liability for a potential human bite.
- Cats — recommended vaccination, not legally mandatory, but strongly recommended, especially for outdoor cats, those living in the countryside, in houses with an attic accessible to martens. Schedule similar to that for dogs.
- Ferrets, exotic farm animals — vaccination available, recommended when in contact with the wild environment. Required for foreign travel (pet passport).
- Humans — pre-exposure prophylaxis (PrEP) recommended for professionally exposed individuals: veterinarians, foresters, hunters, sanitation services, bat researchers. 3-dose schedule, cost 200–400 PLN per dose in the private sector. After PrEP, the post-exposure procedure is shorter and does not require immunoglobulin.
Vaccinating a dog is not just a matter of its health. In the event of a human being bitten by a dog with current proof of vaccination, the doctor may refrain from the full PEP schedule for the victim and recommend 10-day observation of the dog. This is a real difference — five injections and a visit to a rehabilitation center versus a stamp in the dog's health record once a year. If you want to limit contact between pets and martens at all, start with the guide on deterring martens and weasels and the text on recognizing signs of presence.
Untreated rabies = 100% mortality, but in Poland in 2026 it is a rare disease thanks to 30 years of fox vaccinations. Martens get sick sporadically, mainly in areas with active fox outbreaks. Any bite / contact of saliva with cut skin — immediate ER, 15-minute wash, free PEP. Dogs mandatory vaccination, cats recommended, professionally exposed humans — PrEP. Outbreak map: GIWET online.
★Frequently asked questions
Can a marten in Poland have rabies?
Yes, but statistically rarely. A marten is susceptible to infection with the rabies virus just like any other mammal, but it is not a reservoir for the disease in Poland — it is maintained primarily by foxes and raccoon dogs. Out of about 10 cases of rabies detected annually in animals in Poland, over 90% are foxes and raccoon dogs, and martens appear sporadically, once every few years, almost exclusively in areas with an active outbreak among foxes (mainly eastern provinces). A resident of a central or western province can treat the risk as very low, but not zero.
How to recognize a marten sick with rabies?
Diagnosis requires the coexistence of several symptoms, not a single feature. Alarm signals: activity in full sun (martens are nocturnal animals), no flight from humans, lack of coordination, hind leg paralysis, drooling, drooping jaw, aggression without provocation or on the contrary — apathy and disorientation. The daytime activity of an urban stone marten alone does not prove anything. Only the combination of an unusual time, lack of distance from humans, and neurological symptoms requires reporting to the District Veterinary Officer or the 112 emergency number.
What should I do if a marten bit or scratched me?
First: immediately wash the wound with running water and soap for at least 15 minutes, then use an antiseptic (iodine, 70% alcohol, octenidine). Second: immediately report to the ER or a rabies vaccination point (list on the GIS website). Do not wait until the next day. A doctor will assess the exposure category according to WHO and recommend post-exposure prophylaxis — vaccination (5-dose Essen or 4-dose Zagreb scheme) and, if indicated, immunoglobulin. The procedure is free for everyone, regardless of insurance. The decision on PEP is made before symptoms appear — after symptoms, it is too late.
Can my dog catch rabies from a marten?
Theoretically, yes — in an area with an active outbreak, a sick marten could bite a dog and transmit the virus. Practically, the risk is minimized by the mandatory annual vaccination of dogs resulting from Art. 56 of the Animal Health Protection Act. A dog with a current vaccination is practically protected. After a dog is bitten by a wild animal, you should still contact a veterinarian — they may recommend a booster dose and observation. Lack of a current vaccination means that in the event of a bite, the dog will be quarantined with a very serious prognosis.
Does rabies still occur in Poland?
Yes, but on a very limited scale. Poland has been conducting mass oral vaccination of wild foxes since 1993, twice a year, by the Veterinary Inspection and the Polish Hunting Association. As a result, the number of cases dropped from 2,500–3,500 per year in the 1980s to several to a dozen per year in recent years. Since 2013, Poland has had the status of a country territorially free of rabies in wild terrestrial animals according to the WHO/WOAH classification. Individual eastern provinces periodically lose and regain this status. The current map of outbreaks is published by the General Veterinary Inspectorate.
Does pre-exposure prophylaxis (PrEP) make sense for a rural resident?
For most rural residents in Poland, PrEP is not routinely recommended because the risk of exposure in everyday conditions is low, and post-exposure prophylaxis in the event of an incident is free and widely available. PrEP is recommended for individuals with documented increased occupational risk: veterinarians, foresters, hunters, bat researchers, sanitation services, and travelers to countries with endemic rabies. The schedule is 3 doses (days 0, 7, 21, or 28), and the cost in the private sector is 200–400 PLN per dose. After PrEP, the post-exposure procedure is shorter and does not require immunoglobulin — this can also be an argument for people who frequently travel to Asia or Africa.



